Book an appointment
back pain treatment →
Back Pain Over 40 —
Why It Keeps Coming Back
And what actually works to stop the cycle for good.

If you're over 40 and your back pain keeps coming back — just when you thought you'd finally fixed it — you're not imagining things. Back pain in your 40s and 50s behaves differently to the back pain you might have had in your 20s. It tends to linger longer, flare up more easily, and resist the quick fixes that used to work.
Around 4 million Australians (16% of the population) live with back problems, and the burden is highest for people aged 35–54 — the very demographic most likely to be managing work, family, and a body that's quietly changing underneath them. Back problems are the third leading cause of disease burden in Australia, accounting for 4.3% of total disability-adjusted life years lost.
So why does back pain become so persistent after 40? And more importantly — what can actually be done about it?
What Changes in Your Back After 40
Your spine is a remarkable structure, but it isn't immune to the effects of time. Several key changes occur through your 40s and 50s that make back pain both more likely and more stubborn.
Intervertebral disc degeneration is the most well-documented change. The discs between your vertebrae act as shock absorbers, and by age 40, almost everyone has some degree of disc degeneration — even those without symptoms. As discs lose hydration and height, the load on surrounding structures increases. This shifts stress onto the facet joints at the back of the spine, which can develop their own form of arthritis (facet joint syndrome), causing stiffness and a characteristic ache that's often worse in the morning or after sitting for long periods.
Muscle changes compound the problem. From your mid-30s onward, muscle mass naturally declines — a process called sarcopenia — and the deep stabilising muscles of the spine (particularly the multifidus and transversus abdominis) are often the first to lose conditioning, especially after an episode of back pain. Research shows that once these muscles switch off following an injury, they don't automatically switch back on when the pain resolves. This is one of the primary reasons back pain keeps coming back: the pain goes away, but the underlying instability remains.
Lifestyle factors accelerate all of the above. Prolonged sitting — now the norm for most office workers — loads the lumbar spine unevenly and shortens the hip flexors, tilting the pelvis forward and increasing the curve in the lower back. Reduced physical activity, weight gain, and poor sleep all contribute to a cycle where the back becomes progressively more vulnerable to flare-ups from increasingly minor triggers.
"The pain goes away, but the underlying instability remains. That's why it keeps coming back."
Why "Resting It" Makes Things Worse
One of the most persistent myths about back pain is that rest is the best medicine. For acute back pain in your 20s, this might have worked. For persistent back pain over 40, it's often the worst thing you can do.
When you rest, the deep stabilising muscles of your spine continue to weaken. Joints stiffen. The nervous system — which has already been sensitised by repeated pain episodes — becomes even more reactive. What started as a mechanical problem (a strained muscle or irritated joint) can evolve into a sensitised pain state where the nervous system fires pain signals in response to movements and loads that wouldn't normally be painful at all.
This is why so many people over 40 describe their back pain as "unpredictable" — one day they can carry groceries without issue, the next day they bend to pick up a sock and their back goes into spasm. The trigger isn't the sock. It's an underlying system that's been progressively sensitised and destabilised over months or years.
What Evidence-Based Treatment Actually Looks Like
The good news is that persistent back pain over 40 responds very well to the right treatment — and the evidence is clear about what that looks like.
Manual Therapy
Hands-on treatment provided by osteopaths and physiotherapists is effective for reducing pain and improving mobility, particularly in the early stages of a flare-up. Techniques such as spinal mobilisation, soft tissue release, and joint manipulation help restore movement, reduce muscle guarding, and interrupt the pain-spasm cycle. Three months of osteopathic manipulative treatment has been shown to be effective for chronic low back pain, with improved results lasting up to one year.
Targeted Exercise Rehabilitation
This is the most important long-term intervention. This isn't generic gym work — it's a specific, progressive program designed to retrain the deep stabilising muscles of the spine, improve hip and thoracic mobility, and gradually load the structures of the back in a way that builds resilience. The key is having allied health professionals — exercise scientists, physiotherapists, and myotherapists — design and supervise your program, so your training is safe, effective, and built around your injury history.
Education & Load Management
Understanding why your back behaves the way it does — and learning how to manage your activity levels to avoid the boom-bust cycle of overdoing it on good days and being floored on bad days — is a core part of effective treatment. Your osteopath will work with you to identify your specific triggers, modify aggravating activities, and build a sustainable plan for staying active.
The Injury Active Approach: Treat, Rebuild, Prevent
At Injury Active Clinic, we treat back pain differently to most clinics. We don't just treat the episode — we identify and address the underlying reasons it keeps coming back.
Your first appointment includes a thorough assessment of your movement patterns, muscle function, and the specific structures involved in your pain. From there, your osteopath builds a treatment plan that typically combines hands-on treatment with a progressive home exercise program.
For patients who are ready to go beyond pain relief and build lasting strength, our allied health gym at Ravenhall offers a unique step up. Led by exercise scientists, physiotherapists, and myotherapists — with a maximum of 8 people per session — it's designed specifically for people who need to train around an injury or health condition. Every member goes through an in-depth consultation and physical assessment before starting, and programmes are built around your individual goals, movement patterns, and injury history. It's not a standard gym. It's where recovery meets performance.
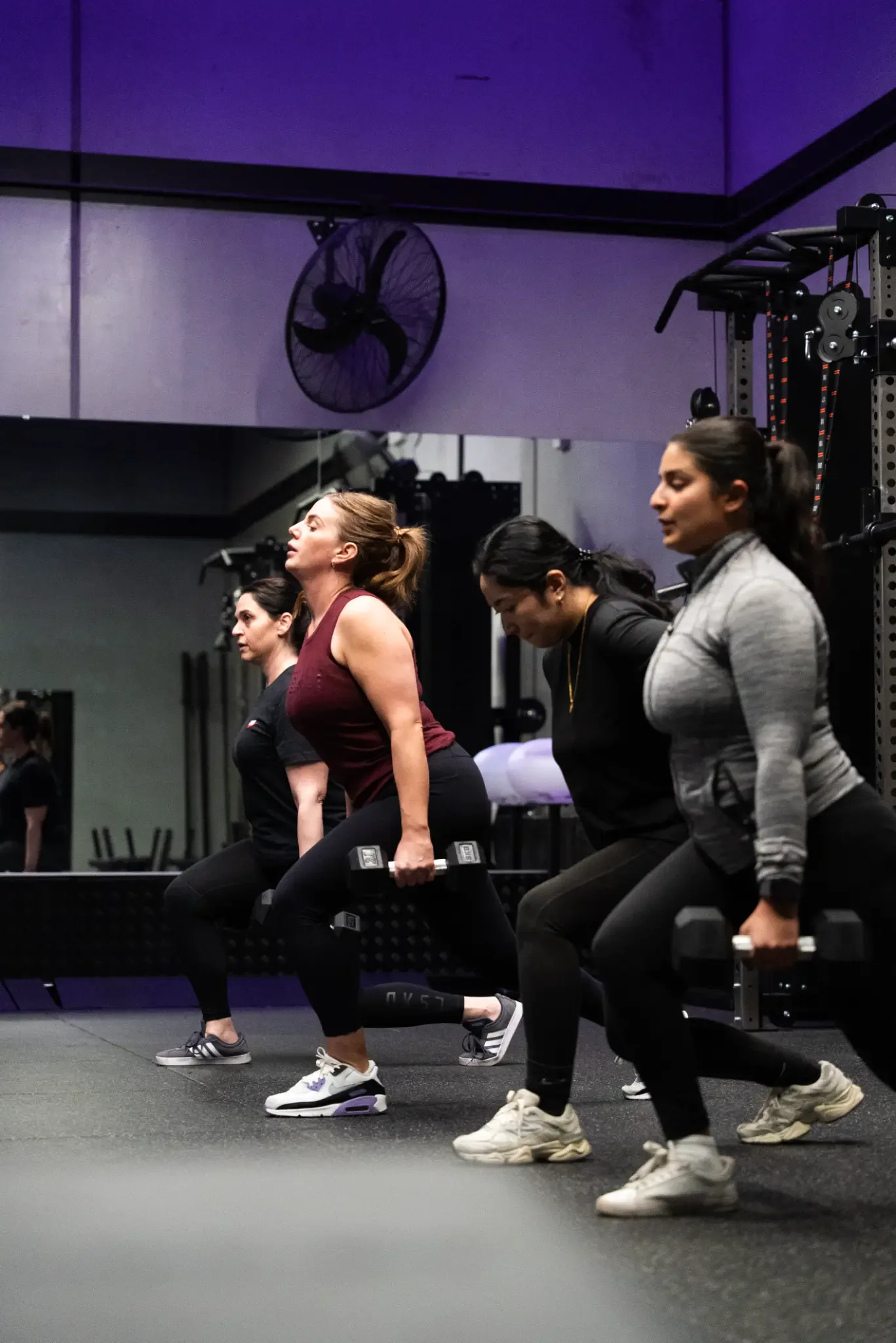
Frequently Asked Questions
How do I know if my back pain is serious?
Most back pain — even severe back pain — is not caused by anything dangerous. However, you should seek urgent assessment if your back pain is accompanied by any of the following: loss of bladder or bowel control, numbness or weakness in both legs, pain following a significant fall or trauma, or unexplained weight loss. If you're unsure, call us and we'll advise you over the phone.
Is osteopathy or physiotherapy better for back pain over 40?
Both osteopathy and physiotherapy are effective for back pain, and the best choice often comes down to the individual practitioner and their approach. At Injury Active Clinic, our osteopaths take a whole-body approach — assessing how your posture, movement patterns, and lifestyle contribute to your pain — and combine hands-on treatment with exercise rehabilitation. We also have physiotherapists available at our Ravenhall clinic.
How many sessions will I need?
This depends on how long you've had the pain and what's driving it. Acute flare-ups often respond within 3–5 sessions. Chronic or recurring back pain typically requires a longer program — 8–12 sessions over 2–3 months — to address the underlying instability and build lasting resilience.
Can I exercise with back pain?
In most cases, yes — and you should. Staying active is one of the most important things you can do for back pain. The key is choosing the right type and intensity of exercise for your current state. Your osteopath will guide you on what's safe and beneficial at each stage of your recovery. For those ready to train more consistently, our allied health gym is designed exactly for this — training that's supervised by clinicians who understand injury.
Will my back pain ever fully resolve?
For many people, yes. With the right treatment and a commitment to the rehabilitation process, it's entirely possible to return to full activity — including sport, heavy lifting, and demanding physical work — without ongoing pain. The goal at Injury Active Clinic is not just to get you out of pain, but to build a back that's strong enough to stay that way.
Ready to Stop
the Cycle?
If your back pain keeps coming back, the answer isn't more rest or more painkillers. It's a proper assessment, a targeted treatment plan, and a commitment to rebuilding the strength your spine needs.
Same-day appointments available · No referral needed · Private health rebates apply
Written by the clinical team at Injury Active Clinic Melbourne. This article is for general information only and does not constitute medical advice. If you are experiencing severe or worsening symptoms, please seek professional assessment.
Get Craig's Weekly
Training & Clinic Update
Every week Craig shares training insights, strength programming notes, clinic updates, and practical advice on managing pain and building long-term fitness. No spam — unsubscribe any time.
Related Articles

Sciatica in Runners: Physiotherapy Tips for Staying Active
When sciatica strikes, it can quickly become one of the most frustrating obstacles in a runner's routine.
Read Article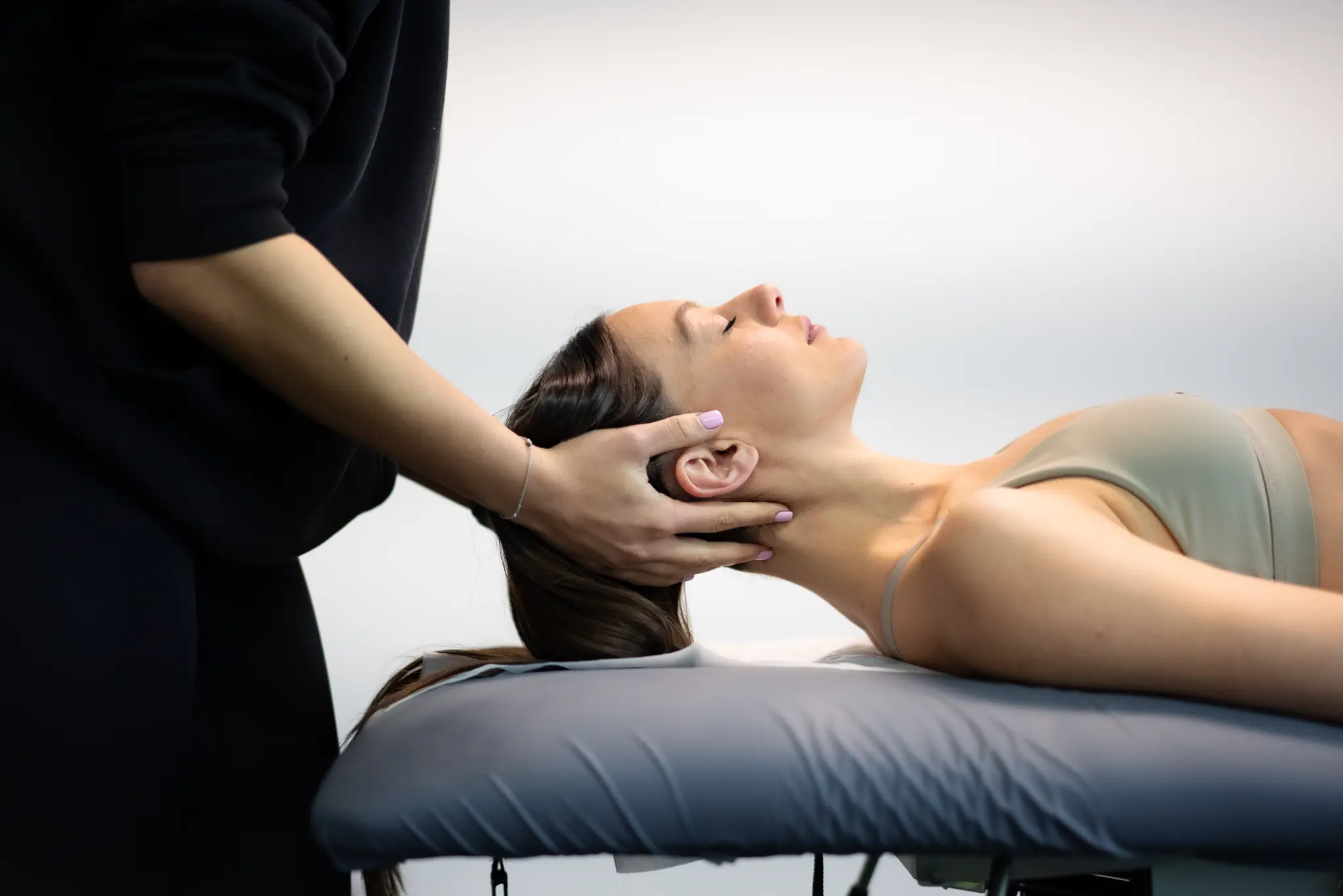
What Is Osteopathy? A Beginner's Guide
Osteopathy focuses on how the body moves and functions. Here's what to expect from your first appointment.
Read Article